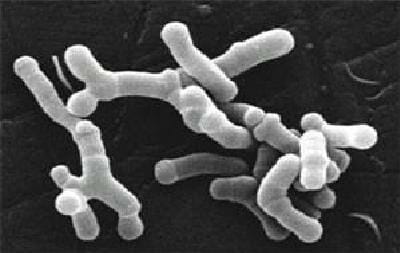
Bifidobacteria is a kind of anaerobic (i.e., lives without oxygen) bacteria that normally inhabit people’s gut and help with food digestion. Bifidobacteria are one of the major genera of bacteria that make up the colon flora in humans and other mammals. One of the most important characteristics of bifidobacteria is that it is considered a probiotic.
The colonization of an infant’s gut is a dynamic process influenced by several factors, such as feeding regimens, medical issues, and microbial presence. Although some commercially available formulas are supplemented with probiotic bacteria, little is known about their ability to modulate an infant’s gut microbial composition and function.
Studying the Role of Bifidobacteria
A group of Germans researchers studied the role of bifidobacteria in a trial titled “Randomized Controlled Trial on the Impact of Early-Life Intervention with Bifidobacteria on the Healthy Infant Fecal Microbiota and Metabolome” (published in The American Journal of Clinical Nutrition), in which they analyzed the impact of infant formula supplemented with four bifidobacterium strains on structural and functional changes in the healthy infant gut from birth through the first year of life.
A total of 117 healthy breastfed, formula-fed, or mixed-fed children were enrolled in the study. The babies were assigned to one of two groups. One group was given a standard whey-based formula enriched with bifidobacteria, and the second group (the control group) was given a formula without bifidobacteria.
Infant stool samples were collected monthly for over a year, preferably in the morning. The samples were taken directly from the diaper and placed into sterile plastic tubes. Then, the samples were frozen and stored until processing. The fecal samples were later analyzed for supplemented bifidobacterium strains using DNA tests and genome comparisons. In addition, the mothers provided a breast milk sample one month after delivery.
In total, 106 babies successfully completed the study, and 70 of them attended a two-year follow-up.
Final Results
The study clearly showed that bifidobacteria supplementation of infant formulas does not substantially affect fecal microbial presence or proportions of bifidobacterial sequences during the first year of life.
In other words, there were no significant differences in the intestinal bacteria populations between the group that received the standard infant formula and the group that received infant formula supplemented with bifidobacteria.
This result differs from the results obtained from adding prebiotics (GOS or FOS) to infant formulas. Adding prebiotics caused a significant increase in the intestinal population of commensal bacteria and thus had beneficial effects.
One interesting result, which further confirms the importance of breastfeeding, is that those children who received more breast milk had a higher amount of bifidobacteria compared to those who only received infant formulas, even if the formula was supplemented with bifidobacteria.
Another important finding was that the intestinal bacteria population of the children who received bifidobacteria-supplemented formula lacked some species that normally should be in the gut. It is suspected that this is a result of a competitive event and bacterial displacement, which might disturb the digestive and immune processes of the child.
In conclusion, although the addition of bifidobacteria to infant formula could increase the microbial population in the gut during the first days of intake, there does not seem to be a long-term impact on the gut microbiota. The effects of changing bacterial and metabolite profiles on human health is unclear and require additional research.
Consult a pediatrician for advice and guidance about feeding a child bifidobacteria-supplemented infant formulas.
Reference
Bazanella, Monika, Tanja V. Maier, Thomas Clavel, Ilias Lagkouvardos, Marianna Lucio, Maria X. Maldonado-Gòmez, Chloe Autran et al. “Randomized Controlled Trial on the Impact of Early-Life Intervention with Bifidobacteria on the Healthy Infant Fecal Microbiota and Metabolome.” The American Journal of Clinical Nutrition 106, no. 5 (2017): 1274–1286. Retrieved from http://ajcn.nutrition.org








